How a wooden bench and an army of grandmothers are helping to lift depression in Zimbabwe and beyond. By Melanie Abas, King’s College London, UK, and Dixon Chibanda, University of Zimbabwe and London School of Hygiene and Tropical Medicine, UK

All over the world and across every culture, millions of people experience feelings of anxiety and depression. What is far less universal is the way in which these feelings are expressed. While the symptoms may be unmistakable, emotional distress finds expression in a myriad of ways across different countries, cultures and communities. Understanding these differences, however, is essential to diagnosing depression and other mental disorders, and can help us to find new and innovative ways to reach those who are suffering.
Lost in translation
[Melanie Abas:] Chiedza was a 26-year-old mother of three living in Harare, Zimbabwe. Her head had been hurting badly for a month so she visited the primary care clinic for help. When the nurse asked if there was anything troubling her, Chiedza’s story came tumbling out. Her eldest child had been sent home from primary school due to unpaid school fees, she explained. ‘What am I supposed to do with the child? I can’t pay her school fees. Sometimes I wash clothes for people for money but, right now, I don't have anything to do. My mind is always occupied. I am not strong. When I am thinking too much I forget, even to cook for the children. My heart feels burdened and I think about how long I will survive like this. Is it better for us just to die?’
There are many people like Chiedza all over the world, for whom a headache can betray a far deeper sense of despair. Depression and anxiety are often debilitating as they interfere with normal brain functioning. Concentration and problem-solving become impaired; anxiety and irritability heighten; one’s mood no longer reacts positively to things that would normally bring a sense of pleasure. Hopelessness and rumination set in.
In 1990, while training as a psychiatrist in London, I undertook a two-year teaching and research position at the University of Zimbabwe Medical School, with funding from the ACU. The economy was stable. Hyperinflation and loss of confidence in the government led by President Mugabe were over a decade away. As part of my research, I worked with a small team – including a fellow trainee, a local psychiatric nurse, and a local social worker ¬– to conduct a series of community-based studies on depression.
In Harare’s city clinics, we found that depressed patients often initially presented with aches and pains. While nurses working on the frontline had the impression that a number of these patients were depressed, they were unsure how to make a diagnosis.
Many of these physical symptoms, especially those related to the heart and the head, were cultural metaphors for fear or grief. But they were often accompanied by two prominent complaints: kufungisisa or ‘thinking too much’ and moyo unorwadza – ‘a painful heavy heart’. Both implied the carrying of an insoluble problem and, together, seemed to encapsulate the experience of depression.
Through interviews with traditional healers and key community figures, we began to establish local terminology for depression. As in many other languages, there are no direct equivalents for depression or anxiety in the Zimbabwean Shona language. But the concept of kufungisisa is used to mean both a cause and a symptom of mental, social, and spiritual distress.
We became the first group to publicise the relevance of the Shona terms kufungisisa and moyo unorwadza as ways in which people often described experiences of anxiety and depression. We proposed that using these terms could help to increase awareness and recognition of mental illness in the community and among primary healthcare providers. We shared our preliminary findings with Vikram Patel, now a leading global mental health researcher, who was starting his own research in Zimbabwe. Vikram went on to develop the Shona Symptom Questionnaire, which was validated as a tool for screening for common mental disorders; it included ‘thinking too much’ as one of its items.
We also developed a tool called the Multiple Symptoms Card to help primary care nurses in Harare detect cases of probable depression. These sorts of ‘task-sharing’ tools – which enable people who are not specialists in mental healthcare to identify and treat symptoms of common mental disorders – are particularly valuable in low and middle income countries, where trained professionals and resources are in short supply. But could this ‘task-sharing’ model be extended even further? And could it work in a community setting, away from the clinics? These were questions being asked by Zimbabwean psychiatrist, Dixon Chibanda, and would eventually lead to our paths crossing.
The Friendship Bench
[Dixon Chibanda:] Shifting forward ten years and Zimbabwe was caught in the throes of political and economic upheaval. In a clinic in Mbare, a high-density and deprived district of Harare, one in three people were suffering from depression. My colleagues and I were asked to develop a primary care mental health programme in Mbare, but there were limitations: it could not take up space inside busy clinics, nor take up the time of over-stretched clinic staff. And it should cost virtually nothing.
Our response – one which would go on to help thousands of people in communities across Africa – was, at its simplest, a wooden bench and an army of trained grandmothers. At the heart of the plan was the idea of teaching people already working in the community how to identify and treat depression. Grandmothers – known as ambuya utanos, who were already providing health education in the community – turned out to be the perfect recruits. The grandmothers volunteered to be trained as counsellors, where they were taught about depression and anxiety and how to diagnose them using the Shona Symptom Questionnaire created by Vikram Patel and the Multiple Symptoms Card developed by Melanie and her team.
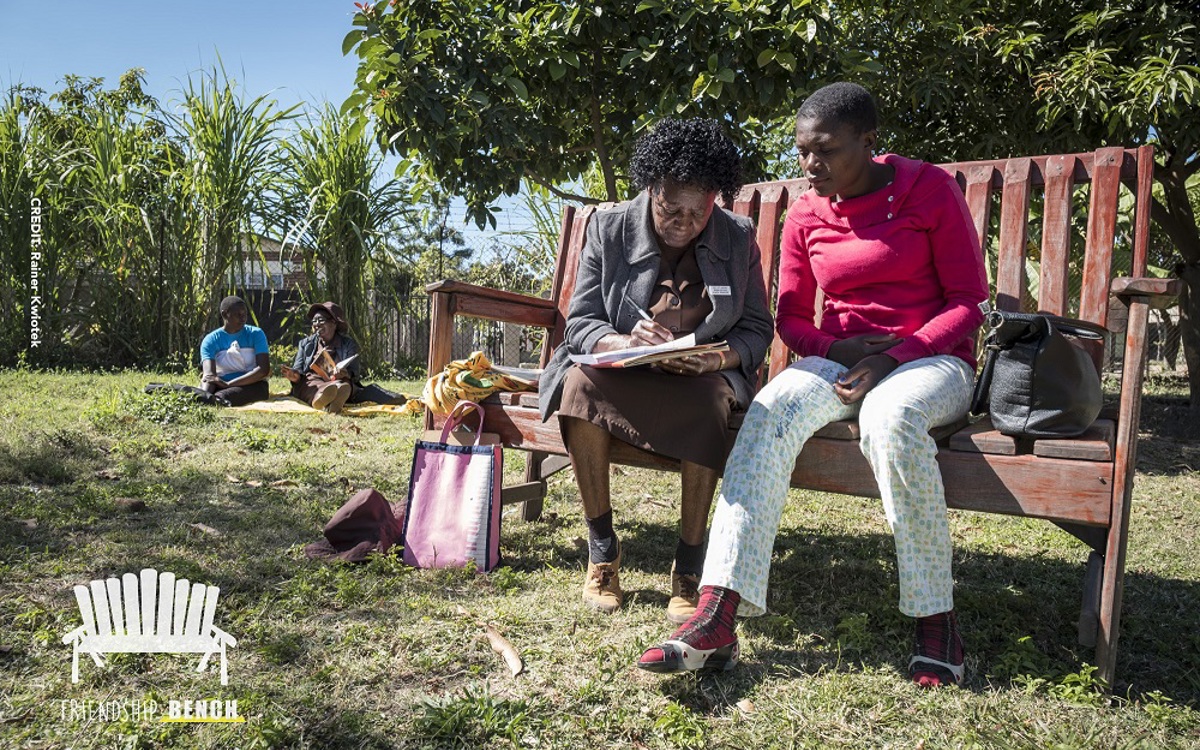
A wooden bench was placed in the clinic grounds on which patients could sit and discuss their problems with the ambuya utano on duty. The ambuya utanos, already rooted in the community, were trained to carry out a structured assessment and provide problem-solving therapy in terms that people could relate to. More severe cases were referred to the primary care clinic. Primary care and community agencies such as the police were invited to refer people to the Friendship Bench, or people could refer themselves.
Since its first outing in 2006, the Friendship Bench programme has been refined and expanded, but the fundamental concept remains the same. A critical milestone was the publication of results from a randomised controlled trial of the programme, funded by Grand Challenges Canada, showing its effectiveness in treating common mental disorders. Today, ambuyas are supervised by district health promotion officers with the help of training manuals produced by Dr Ruth Verhey. The team, including Dr Verhey and Dr Tarisai Bere, have trained more than 600 grandmothers in evidence-based talking therapy, which they deliver for free in more than 70 communities in Zimbabwe.

In 2017 alone, 30,000 people visited a Friendship Bench. The programme has expanded beyond Zimbabwe, to Malawi, Zanzibar, and even New York City, highlighting that interventions created in low and middle income countries can be adapted for high income ones too.
The programme’s core values are ‘empathy and connection, anchored in research’. The evidence-based research which underpinned this intervention was vital in proving its effectiveness, which in turn gave policymakers the confidence to expand it to reach more people.
While much of the academic support initially came from UK universities, such King’s College London and the London School of Hygiene and Tropical Medicine, we have since turned that around. Today, many of the local Friendship Bench team members have started or completed PhDs; I lead the African Mental Health Research Initiative – a consortium of four African universities working with UK institutions to build an Africa-led network of researchers in mental health. Together, universities have a critical role to play in forming long-term partnerships across the globe, bridging communities and countries, with the potential for all to be enriched. To quote an African proverb used by the Friendship Bench team: if you want to go fast, go alone. If you want to go far, go together.
Melanie Abas is Professor of Global Mental Health at the Institute of Psychiatry, Psychology and Neuroscience, King’s College London, UK, and Deputy Director of the Centre for Global Mental Health.
Dr Dixon Chibanda is Director of the African Mental Health Research Initiative at the University of Zimbabwe, and Associate Professor of Global Mental Health at the London School of Hygiene and Tropical Medicine, UK.
To find out more about the Friendship Bench, visit www.friendshipbenchzimbabwe.org
Images by Rainer Kwiotek, courtesy of the Friendship Bench
